Emergency Dental Care of New York
Contact
Hours
- Monday: 9:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 9:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Emergency Dental Care, located in the bustling city of New York, New York, is your trusted provider of urgent dental services when unexpected dental issues arise. Dedicated to providing prompt relief and comprehensive care for dental emergencies, our practice offers a wide range of immediate treatment options in a welcoming and comfortable environment. Led by a team of experienced emergency dentists, Emergency Dental Care is committed to restoring your oral health and relieving your discomfort as quickly as possible.
Urgent Dental Services
Emergency Examinations
- Immediate Assessments: Thorough evaluations to diagnose and address dental emergencies promptly.
- Pain Management: Quick relief from dental pain through effective anesthesia and pain management techniques.
Emergency Dental Treatments
- Emergency Extractions: Prompt removal of severely damaged or infected teeth causing acute pain or discomfort.
- Emergency Root Canal Therapy: Expedited root canal treatment to alleviate pain and save infected teeth.
Immediate Care
Same-Day Appointments
- Flexible Scheduling: Accommodating same-day appointments for patients in need of urgent dental care.
- Walk-In Services: Convenient walk-in availability for immediate assessment and treatment of dental emergencies.
Efficient Treatment
- Rapid Response: Prompt attention from skilled emergency dentists to address urgent dental needs without delay.
- Streamlined Procedures: Expedited processes to minimize waiting times and efficiently manage dental emergencies.
Patient Care
Compassionate Approach
- Empathetic Staff: Compassionate and understanding dental professionals dedicated to providing comfort and support during stressful situations.
- Clear Communication: Transparent communication about treatment options, costs, and expectations to empower patients to make informed decisions about their dental care.
Aftercare Support
- Post-Treatment Guidance: Detailed instructions and guidance on post-procedure care and pain management to promote optimal healing and recovery.
- Follow-Up Care: Scheduled follow-up appointments to monitor progress, address any concerns, and ensure the successful resolution of dental emergencies.
Malocclusion
Malocclusion refers to misalignment or incorrect positioning of the teeth when the jaws are closed. It can manifest in various forms, affecting the way the upper and lower teeth fit together, also known as occlusion. Malocclusion may result from genetic factors, developmental issues, habits, or injuries, and it can lead to problems with chewing, speech, and oral health.
Here are some key points about malocclusion:
- Types: Malocclusion can present in different forms, including:
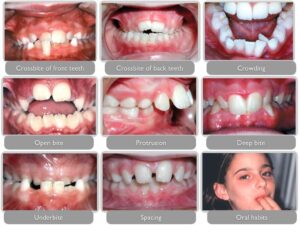
- Overbite: The upper front teeth excessively overlap the lower front teeth vertically.
- Underbite: The lower front teeth protrude forward beyond the upper front teeth, creating an abnormal bite.
- Crossbite: One or more upper teeth sit inside the lower teeth rather than outside when the jaws are closed.
- Open bite: There is a space between the upper and lower front or side teeth when the jaws are closed, preventing them from meeting properly.
- Crowding: Insufficient space in the dental arch causes teeth to overlap or become crooked.
- Spacing: Excessive gaps or spaces between teeth due to missing teeth or abnormal growth.
- Misalignment: Teeth may be rotated, tilted, or displaced from their proper positions within the dental arch.
- Causes:
- Genetics: Malocclusion can run in families, indicating a genetic predisposition to certain dental and jaw traits.
- Developmental factors: Irregular tooth eruption, abnormal growth of the jawbones, or facial trauma during childhood can contribute to malocclusion.
- Oral habits: Thumb sucking, tongue thrusting, prolonged pacifier use, or mouth breathing can affect dental and facial development, leading to malocclusion.
- Dental conditions: Early loss of primary (baby) teeth, impacted teeth, or dental restorations that alter tooth alignment can cause malocclusion.
- Skeletal abnormalities: Abnormal growth patterns or structural anomalies of the jawbones can result in malocclusion.
- Symptoms:
- Difficulty biting or chewing food properly.
- Speech problems, such as lisping or difficulty pronouncing certain sounds.
- Jaw pain, discomfort, or tension.
- Temporomandibular joint (TMJ) disorders, including clicking, popping, or locking of the jaw.
- Uneven wear of tooth surfaces or premature tooth wear.
- Self-consciousness about the appearance of the smile or facial profile.
- Diagnosis:
- Diagnosis of malocclusion involves a comprehensive dental examination, which may include:
- Visual assessment of tooth alignment, jaw relationship, and facial symmetry.
- Dental impressions, X-rays, or digital scans to evaluate tooth and jaw relationships more precisely.
- Bite analysis to assess occlusal discrepancies and functional issues during jaw movement.
- Treatment:
- Treatment options for malocclusion depend on the type and severity of the condition, as well as the individual's age and oral health needs. Treatment may include:
- Orthodontic treatment: Braces, clear aligners, or other orthodontic appliances are used to move teeth into their proper positions and correct bite discrepancies.
- Tooth extractions: In cases of severe crowding, impacted teeth, or skeletal discrepancies, extractions may be necessary to create space or facilitate orthodontic treatment.
- Jaw surgery (orthognathic surgery): For significant skeletal malocclusion or jaw misalignment, surgical intervention may be required to reposition the jaws and achieve proper occlusion.
- Dental restorations: Crowns, veneers, or dental implants may be used to restore tooth alignment, improve aesthetics, and enhance occlusal function.
- Oral appliances: In some cases, removable or fixed appliances may be prescribed to address specific functional or developmental issues, such as thumb sucking or tongue thrusting.
In summary, malocclusion refers to misalignment or incorrect positioning of the teeth and jaws when the mouth is closed. It can manifest in various forms and may result from genetic factors, developmental issues, habits, or injuries. Malocclusion can lead to problems with chewing, speech, and oral health, but it can often be successfully treated with orthodontic interventions, dental restorations, or surgical procedures, depending on the individual's needs and the severity of the condition. Early diagnosis and appropriate treatment are essential for addressing malocclusion and improving oral function, aesthetics, and overall well-being.
Ridge Augmentation
Ridge augmentation is a dental procedure used to rebuild or augment the bone in the jaw ridge (alveolar ridge) to restore its natural shape and volume. This procedure is typically performed to prepare the jawbone for dental implant placement or to improve the aesthetics and function of the jaw in cases of bone loss or deformity. Here's an overview of ridge augmentation:
- Indications:
- Ridge augmentation may be indicated when there is insufficient bone volume or density in the jaw ridge to support dental implants or maintain proper function and aesthetics.
- It may be necessary following tooth extraction, especially if the extraction site lacks adequate bone volume or if bone resorption has occurred over time.
- Ridge augmentation can also be used to correct deformities or irregularities in the jaw ridge caused by trauma, congenital defects, or periodontal disease.
- Preparation:
- Before performing ridge augmentation, the dentist or oral surgeon will conduct a comprehensive evaluation of the patient's oral health and assess the bone volume and quality using radiographic imaging (such as dental X-rays or CBCT scans).
- Depending on the extent of bone loss or deformity, additional diagnostic tests or procedures may be required to plan the augmentation procedure effectively.
- Procedure:
- Ridge augmentation can be performed using various techniques and materials, including bone grafts, bone substitutes, and guided bone regeneration (GBR) procedures.
- During the procedure, the dentist or oral surgeon makes an incision in the gum tissue to access the underlying bone and create space for the bone graft material.
- The bone graft material, which may be harvested from the patient's own body (autograft), obtained from a tissue bank (allograft), or synthetic (alloplastic), is placed in the defect or augmentation site.
- Barrier membranes or collagen membranes may be used to cover the graft material and promote new bone growth while preventing soft tissue ingrowth.
- The incision is then closed with sutures, and the graft site is allowed to heal over several months.
- Postoperative Care:
- After ridge augmentation, the patient may experience some discomfort, swelling, or minor bleeding in the surgical area. Pain medication and cold compresses may be recommended to alleviate discomfort and reduce swelling.
- The patient should follow postoperative instructions provided by the dentist or oral surgeon, including dietary restrictions, oral hygiene practices, and any prescribed medications.
- Healing typically occurs over several months as new bone forms and integrates with the existing bone.
- Follow-up:
- Follow-up appointments may be scheduled to monitor healing and assess the success of the ridge augmentation.
- Once adequate bone volume and density have been restored, the jaw ridge may be ready for dental implant placement or other restorative procedures.
- Regular dental check-ups and professional cleanings are important for maintaining oral health and monitoring the long-term stability of the augmented ridge.
Ridge augmentation is a valuable procedure for restoring bone volume and shape in the jaw ridge, enabling successful dental implant placement and improving oral function and aesthetics. If you are considering ridge augmentation or dental implant treatment, it's important to consult with a qualified dental professional for an evaluation and personalized treatment plan tailored to your specific needs.