Barnet Health Doctors
Contact
Hours
<ul id=”hours” style=”transition: height .3s ease;”>
<li>Monday: 9:00am – 9:00pm</li>
<li>Tuesday: 9:00am – 6:00pm</li>
<li>Wednesday: 9:00am – 9:00pm</li>
<li>Thursday: 9:00am – 9:00pm</li>
<li>Friday: 9:00am – 5:00pm</li>
</ul>
Barnet Health Doctors, nestled in the picturesque town of Livingston Manor, New York, is a premier dental institution committed to delivering top-notch dental care to patients in the community. With a dedication to excellence and patient satisfaction, the practice offers a wide range of dental services designed to promote oral health and enhance smiles. Led by a team of experienced dental professionals, Barnet Health Doctors provides personalized care in a comfortable and welcoming environment.
Dental Services
Preventive Dentistry
- Comprehensive Examinations: Thorough dental check-ups to assess oral health and detect any signs of dental issues.
- Professional Cleanings: Routine cleanings to remove plaque and tartar buildup, preventing gum disease and cavities.
- Dental Sealants: Protective coatings applied to the chewing surfaces of molars to prevent decay, especially in children.
Restorative Dentistry
- Fillings: Treatment of cavities with tooth-colored composite fillings for a natural-looking restoration.
- Crowns and Bridges: Custom-made dental crowns and bridges to restore and strengthen damaged or missing teeth.
- Dental Implants: Permanent tooth replacement option that looks, feels, and functions like natural teeth.
Specialized Dental Care
Orthodontics
- Braces: Traditional metal braces and clear aligner therapy to correct misaligned teeth and bite issues.
- Retainers: Custom-fitted retainers to maintain the results of orthodontic treatment and prevent teeth from shifting.
Endodontics
- Root Canal Therapy: Treatment to save and repair infected or damaged teeth by removing infected pulp and sealing the root canal.
- Apicoectomy: Surgical procedure to remove the tip of the tooth root and seal the root canal to treat persistent infections.
Patient Care
Personalized Treatment Plans
- Individualized Consultations: Detailed discussions and treatment planning sessions to address each patient’s unique dental needs and goals.
- Collaborative Approach: Working closely with patients to develop treatment plans that align with their preferences and budget.
Comfort and Convenience
- Relaxing Environment: Creating a comfortable and welcoming atmosphere to ensure patients feel at ease during their dental visits.
- Pain Management: Utilizing gentle techniques and advanced anesthesia options to minimize discomfort during procedures.
Halitosis
Halitosis, commonly known as bad breath, is a condition characterized by unpleasant odors emanating from the mouth. It can be temporary or persistent and may be caused by various factors, including poor oral hygiene, dietary habits, medical conditions, or lifestyle factors. Halitosis can lead to social discomfort, embarrassment, and may indicate underlying oral health issues that require attention.
Here are some key points about halitosis:
- Causes:
- Poor oral hygiene: Inadequate brushing, flossing, and tongue cleaning can lead to the accumulation of food particles, bacteria, and plaque in the mouth, contributing to halitosis.
- Oral infections: Gum disease (periodontitis), tooth decay, or oral infections such as oral thrush can produce foul-smelling gases and contribute to bad breath.
- Dry mouth: Reduced saliva flow, often caused by medications, medical conditions, or mouth breathing, can lead to dry oral tissues and an increased risk of halitosis.
- Dietary factors: Certain foods and beverages, such as garlic, onions, spicy foods, coffee, and alcohol, contain volatile compounds that can linger in the mouth and cause bad breath.
- Tobacco use: Smoking or using tobacco products can lead to dry mouth, gum disease, and oral infections, all of which contribute to halitosis.
- Medical conditions: Underlying medical conditions such as respiratory infections, sinusitis, gastroesophageal reflux disease (GERD), diabetes, liver or kidney disease, or certain cancers can cause halitosis.
- Lifestyle factors: Stress, fasting, crash dieting, or certain dietary supplements can affect breath odor and contribute to halitosis.
- Symptoms:
- Persistent bad breath that does not improve with oral hygiene measures.
- Unpleasant taste or dryness in the mouth.
- White or yellowish coating on the tongue.
- Dry, sticky oral tissues.
- Postnasal drip or throat discomfort in cases of halitosis related to sinusitis or respiratory infections.
- Mouth sores, bleeding gums, or other signs of oral infections or gum disease.
- Diagnosis:
- Diagnosis of halitosis typically involves a comprehensive oral examination, medical history review, and assessment of oral hygiene practices and dietary habits.
- Your dentist or healthcare provider may inquire about symptoms, lifestyle factors, and any underlying medical conditions that could contribute to bad breath.
- Additional tests, such as measurement of saliva flow rate, assessment of gum health, or bacterial analysis of oral samples, may be conducted to identify the underlying cause of halitosis.
- Treatment:
- Treatment of halitosis aims to address the underlying cause and alleviate symptoms. Treatment options may include:
- Improving oral hygiene: Practicing good oral hygiene habits, including regular brushing, flossing, and tongue cleaning, can help reduce bacteria and plaque accumulation and improve breath odor.
- Treating oral infections: Addressing gum disease, tooth decay, or oral infections with professional dental cleanings, periodontal therapy, or restorative treatments can help eliminate sources of bad breath.
- Managing dry mouth: Staying hydrated, using saliva substitutes, or adjusting medications that contribute to dry mouth can help alleviate symptoms of halitosis related to reduced saliva flow.
- Dietary modifications: Limiting consumption of odor-causing foods and beverages and maintaining a balanced diet can help reduce breath odor.
- Quitting smoking or tobacco use: Stopping smoking or using tobacco products can improve oral health and reduce halitosis.
- Treating underlying medical conditions: Managing underlying medical conditions such as sinusitis, GERD, diabetes, or respiratory infections can help alleviate halitosis symptoms.
- Prevention:
- To prevent halitosis, it's important to:
- Maintain good oral hygiene practices, including regular brushing, flossing, and tongue cleaning.
- Drink plenty of water throughout the day to stay hydrated and promote saliva flow.
- Limit consumption of odor-causing foods and beverages, and practice moderation with alcohol and tobacco.
- Visit your dentist regularly for professional cleanings and oral examinations to detect and treat oral health problems early.
- Address underlying medical conditions or lifestyle factors that may contribute to halitosis, such as dry mouth, sinusitis, or tobacco use.
In summary, halitosis is a common condition characterized by unpleasant odors emanating from the mouth. It can be caused by various factors, including poor oral hygiene, oral infections, dry mouth, dietary habits, medical conditions, or lifestyle factors. Treatment of halitosis aims to address the underlying cause and alleviate symptoms through measures such as improving oral hygiene, treating oral infections, managing dry mouth, and addressing underlying medical conditions. If you experience persistent bad breath or halitosis symptoms, it's important to consult your dentist or healthcare provider for evaluation and appropriate treatment.
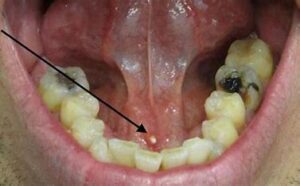
Salivary Gland Stones
Salivary gland stones, also known as sialoliths or salivary calculi, are calcified deposits that form within the ducts of the salivary glands. These stones can block the flow of saliva from the gland into the mouth, leading to symptoms such as pain, swelling, and difficulty eating or opening the mouth.
Here are some key points about salivary gland stones:
- Formation: Salivary gland stones typically form when minerals in saliva (such as calcium and phosphate) crystallize and accumulate within the ducts of the salivary glands. The exact cause of stone formation is not always clear but may be related to factors such as dehydration, reduced salivary flow, bacterial infection, or structural abnormalities of the salivary ducts.
- Location: Salivary gland stones most commonly occur in the ducts of the submandibular glands, which are located beneath the floor of the mouth. However, they can also affect the ducts of the parotid glands (located in the cheeks) or the sublingual glands (located beneath the tongue).
- Symptoms: The presence of a salivary gland stone can cause symptoms such as pain and swelling in the affected gland, particularly during meals when saliva production increases. Other symptoms may include difficulty opening the mouth, dry mouth, foul-tasting saliva, or recurrent infections (sialadenitis) due to obstruction of the gland's duct.
- Diagnosis: Diagnosis of salivary gland stones typically involves a combination of medical history, physical examination, and imaging studies. Imaging tests such as ultrasound, CT scan, or sialography (a specialized X-ray procedure) may be used to visualize the location and size of the stone within the salivary duct.
- Treatment: Treatment of salivary gland stones depends on the size and location of the stone, as well as the severity of symptoms. Small stones may be managed conservatively with measures such as hydration, warm compresses, sour candies, or massage to stimulate saliva flow and facilitate stone expulsion. Larger stones or stones causing persistent symptoms may require more invasive treatment, such as manual expression of the stone, sialendoscopy (insertion of a tiny endoscope into the duct to visualize and remove the stone), or surgical removal of the affected gland (sialadenectomy).
- Prevention: To prevent the formation of salivary gland stones, it is important to maintain good oral hygiene, stay well-hydrated, and avoid risk factors such as dehydration, reduced salivary flow, or poor dietary habits that may contribute to stone formation. Regular dental check-ups and prompt treatment of any underlying conditions that may predispose to stone formation can also help prevent recurrence.
In summary, salivary gland stones are calcified deposits that form within the ducts of the salivary glands, leading to symptoms such as pain, swelling, and difficulty eating. Treatment options vary depending on the size and location of the stone but may include conservative measures, minimally invasive procedures, or surgical intervention to alleviate symptoms and prevent complications.