Invisalign Center of NYC
The Invisalign Center of NYC, located in the bustling city of New York, is a premier destination for state-of-the-art orthodontic treatment. Specializing in Invisalign clear aligner therapy, the center offers a modern and convenient approach to achieving straighter teeth and a confident smile. Patients at the Invisalign Center of NYC receive personalized care from a team of skilled orthodontic professionals dedicated to delivering outstanding results.
Orthodontic Services
Invisalign Treatment
- Customized Treatment Plans: Each patient receives a personalized treatment plan tailored to their unique orthodontic needs and smile goals.
- Advanced Technology: Utilizing cutting-edge digital scanning technology to create precise 3D models of the teeth for custom Invisalign aligners.
- Transparent Aligners: Invisalign clear aligners are virtually invisible, providing a discreet and comfortable orthodontic solution.
Comprehensive Care
- Initial Consultation: Thorough examination and discussion of treatment options to determine if Invisalign is the right choice for the patient.
- Progress Monitoring: Regular check-ups to monitor progress and ensure the treatment is progressing as planned.
- Refinements: Fine-tuning the treatment plan as needed to achieve the desired results.
Patient Experience
Convenience and Comfort
- Flexible Appointments: Accommodating scheduling options to fit the busy lifestyles of patients in the heart of NYC.
- Virtual Consultations: Convenient online consultations for initial assessments and treatment planning.
- Comfortable Treatment: Invisalign aligners are smooth and comfortable to wear, with no sharp edges or wires to cause irritation.
Educational Resources
- Smile Simulation: Utilizing advanced software to provide patients with a preview of their smile transformation before starting treatment.
- Oral Hygiene Guidance: Education on proper oral hygiene practices to maintain healthy teeth and gums during treatment.
- Supportive Team: A team of knowledgeable and caring orthodontic professionals available to answer questions and provide guidance throughout the treatment process.
All-on-4 Dental Implants
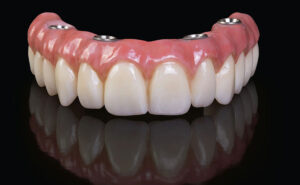
"All-on-4" dental implants refer to a specific dental implant treatment concept designed to provide edentulous (toothless) patients with a fixed full-arch dental restoration supported by only four dental implants. This innovative treatment approach allows for the rehabilitation of an entire dental arch (either upper or lower) using fewer implants compared to traditional implant-supported prostheses. Here's an overview of the All-on-4 dental implant procedure:
- Evaluation and Treatment Planning:
- Before undergoing All-on-4 dental implant treatment, the patient will undergo a comprehensive dental examination, including clinical assessment and radiographic evaluation (such as dental X-rays or CBCT scans).
- The dentist or oral surgeon will assess the patient's oral health, bone density, and suitability for implant placement.
- A detailed treatment plan will be developed based on the patient's individual needs and goals.
- Implant Placement:
- The first step in the All-on-4 dental implant procedure involves surgically placing four dental implants into the jawbone at strategic locations to support the full-arch restoration.
- The implants are strategically angled and positioned to maximize bone anchorage and avoid anatomical structures, such as nerves or sinuses.
- Implant placement is typically performed under local anesthesia or sedation to ensure the patient's comfort during the procedure.
- Immediate Loading:
- In many cases, All-on-4 dental implants allow for immediate loading, meaning that a temporary fixed prosthesis can be attached to the implants on the same day as surgery.
- Immediate loading provides patients with immediate function and aesthetics while the implants undergo osseointegration.
- Healing and Osseointegration:
- After implant placement, a healing period of several months is usually required to allow for osseointegration to occur.
- During this time, the implants fuse with the surrounding bone tissue, becoming firmly anchored in the jawbone.
- Temporary restorations may be placed during the healing period to maintain aesthetics and function.
- Final Restoration:
- Once osseointegration is complete, the dental implants are ready to support the final full-arch restoration.
- A custom-made fixed prosthesis, typically made of high-quality dental materials such as porcelain or acrylic, is fabricated to fit securely over the implants and restore function and aesthetics.
- The final prosthesis is attached to the implants using special abutments or connectors, providing stability and support for chewing and speaking.
- Postoperative Care and Maintenance:
- After the All-on-4 dental implant restoration is placed, the patient will receive instructions on postoperative care and maintenance.
- Regular dental check-ups and professional cleanings are essential to monitor the health of the implants and surrounding tissues.
- Good oral hygiene practices, including brushing, flossing, and using antimicrobial mouthwash, are important for long-term success.
All-on-4 dental implants offer several advantages over traditional removable dentures, including improved stability, function, and aesthetics. With proper care and maintenance, an All-on-4 dental implant restoration can provide long-lasting and natural-looking results, enhancing both oral health and quality of life. If you are considering All-on-4 dental implant treatment, it's important to consult with a qualified dental professional to determine the best treatment plan for your individual needs.
Dry Mouth
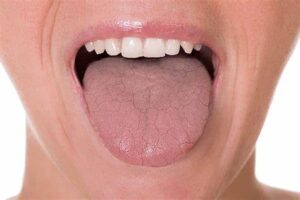
Dry mouth, also known as xerostomia, is a condition characterized by a decrease in saliva production or a change in the composition of saliva. Saliva plays a crucial role in maintaining oral health by lubricating the mouth, neutralizing acids, washing away food particles, and aiding in digestion and speech. Reduced saliva flow can lead to discomfort, difficulty eating and speaking, and an increased risk of dental problems such as tooth decay and gum disease.
Here are some key points about dry mouth:
- Causes:
- Medications: Dry mouth is a common side effect of many prescription and over-the-counter medications, including antihistamines, decongestants, antidepressants, antipsychotics, and certain blood pressure medications.
- Medical conditions: Systemic diseases such as Sjögren's syndrome, diabetes, HIV/AIDS, Parkinson's disease, and autoimmune disorders can affect salivary gland function and lead to dry mouth.
- Radiation therapy: Treatment for head and neck cancer involving radiation to the head and neck area can damage the salivary glands and reduce saliva production.
- Chemotherapy: Some chemotherapy drugs can cause temporary or permanent damage to the salivary glands, leading to dry mouth.
- Aging: Salivary gland function tends to decrease with age, leading to a higher prevalence of dry mouth in older adults.
- Mouth breathing: Breathing through the mouth, particularly during sleep, can dry out the oral tissues and contribute to dry mouth symptoms.
- Smoking or tobacco use: Tobacco use can decrease saliva production and exacerbate dry mouth symptoms.
- Symptoms:
- Dry, sticky feeling in the mouth or throat.
- Difficulty chewing, swallowing, or speaking.
- Persistent thirst.
- Sore throat or hoarseness.
- Dry or cracked lips.
- Bad breath (halitosis).
- Changes in taste or difficulty tasting food.
- Increased risk of oral infections, tooth decay, or gum disease.
- Difficulty wearing dentures or oral appliances due to lack of saliva lubrication.
- Complications:
- Oral health problems: Reduced saliva flow can lead to an increased risk of cavities, gum disease, oral infections (such as thrush), and oral sores or ulcers.
- Difficulty eating and speaking: Dry mouth can make it challenging to chew and swallow food, leading to nutritional deficiencies or weight loss. It can also affect speech clarity and articulation.
- Decreased quality of life: Chronic dry mouth can impact oral comfort, social interactions, and overall well-being, leading to decreased quality of life and psychological distress.
- Diagnosis:
- Diagnosis of dry mouth is based on patient symptoms, medical history, and clinical evaluation by a healthcare professional.
- Your healthcare provider may inquire about medication use, medical conditions, lifestyle factors, and oral hygiene habits that could contribute to dry mouth.
- Additional tests, such as salivary flow rate measurement or blood tests, may be conducted to assess salivary gland function and identify underlying causes of dry mouth.
- Treatment:
- Treatment of dry mouth aims to alleviate symptoms, stimulate saliva production, and prevent complications. Treatment options may include:
- Hydration: Drinking plenty of water or sugar-free fluids throughout the day can help keep the mouth moist and relieve dry mouth symptoms.
- Saliva substitutes: Over-the-counter or prescription saliva substitutes, gels, sprays, or mouth rinses can provide temporary relief by lubricating the mouth and mimicking the properties of natural saliva.
- Salivary stimulants: Chewing sugar-free gum or sucking on sugar-free candies can stimulate saliva production and increase saliva flow.
- Medication adjustment: Your healthcare provider may adjust or change medications that contribute to dry mouth symptoms, if possible.
- Oral hygiene: Maintaining good oral hygiene practices, including regular brushing, flossing, and dental check-ups, can help prevent oral health problems associated with dry mouth.
- Humidification: Using a humidifier in the bedroom or living space can add moisture to the air and help reduce dry mouth symptoms, particularly during sleep.
- Prevention:
- To prevent or minimize dry mouth symptoms, it's important to:
- Stay hydrated by drinking plenty of water throughout the day.
- Avoid or limit alcohol, caffeine, and tobacco, which can contribute to dry mouth.
- Use a humidifier in dry indoor environments to add moisture to the air.
- Practice good oral hygiene habits, including regular brushing, flossing, and dental check-ups.
- Chew sugar-free gum or suck on sugar-free candies to stimulate saliva flow.
- Avoid mouthwashes containing alcohol, as they can exacerbate dry mouth symptoms.
In summary, dry mouth is a common condition characterized by reduced saliva production or changes in saliva composition. It can result from various factors, including medications, medical conditions, radiation therapy, and aging. Dry mouth can lead to discomfort, difficulty eating and speaking, and an increased risk of oral health problems. Treatment options for dry mouth aim to alleviate symptoms, stimulate saliva production, and prevent complications. If you experience persistent or severe dry mouth symptoms, it's important to consult a healthcare professional for evaluation and appropriate management.