Stony Brook Medicine
Contact
Hours
- Monday: 9:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 9:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Stony Brook Medicine, located in Stony Brook, New York, is a renowned healthcare institution providing a wide array of medical and dental services. Known for its state-of-the-art facilities and cutting-edge technology, Stony Brook Medicine is staffed by a dedicated team of highly trained animal medical professionals committed to delivering compassionate and innovative care to all patients.
Medical Services
General Medicine and Surgery
- Emergency Services: Available 24/7, featuring the latest emergency medical technology and highly skilled animal medical personnel.
- Inpatient and Outpatient Care: Comprehensive services including internal medicine, cardiology, neurology, orthopedics, and more.
- Robotic Surgery: Advanced minimally invasive procedures using cutting-edge robotic technology for precision and faster recovery times.
Specialized Departments
- Rheumatology: Expert care for arthritis, autoimmune diseases, and musculoskeletal disorders.
- Dermatology: Comprehensive treatment for skin conditions, including eczema, psoriasis, and skin cancer.
- Pulmonology: Advanced care for respiratory conditions, including asthma, COPD, and lung infections.
- Geriatrics: Specialized care for elderly patients, focusing on maintaining health, independence, and quality of life.
Dental Services
General Dentistry
- Preventive Care: Routine checkups, cleanings, and education to maintain oral health.
- Sealants and Fluoride Treatments: Protective treatments to prevent decay, especially in children.
Specialized Dental Care
- Oral and Maxillofacial Pathology: Diagnosis and treatment of diseases affecting the oral and maxillofacial regions.
- Implant Dentistry: Expert placement of dental implants to replace missing teeth and restore functionality.
- Periodontics: Advanced treatment for gum diseases and other conditions affecting the tissues surrounding the teeth.
- Orthodontics: Comprehensive orthodontic treatments for children and adults to correct dental alignment and bite issues, including braces and clear aligners.
- Sleep Dentistry: Specialized care for dental issues related to sleep disorders, such as sleep apnea.
Oral Lichen Planus
Oral lichen planus (OLP) is a chronic inflammatory condition that affects the mucous membranes inside the mouth. It is believed to be an autoimmune disorder, where the body's immune system mistakenly attacks the cells of the oral mucosa, leading to inflammation and the development of characteristic lesions.
Here are some key points about oral lichen planus:
- Symptoms: OLP typically presents with various symptoms, which may include:
- White, lacy patches (reticular lesions) on the inside of the cheeks, tongue, or gums.
- Red, swollen patches (erythematous lesions) or ulcers in the mouth.
- Burning sensation or discomfort, particularly when consuming spicy or acidic foods.
- Pain or sensitivity to hot, cold, or spicy foods.
- Dry mouth (xerostomia) or altered taste sensation (dysgeusia).
- Clinical Presentation: Oral lichen planus lesions can vary in appearance and may manifest as:
- Reticular lesions: Fine, white lines or lacy patches that may intersect and form a network-like pattern.
- Erosive or ulcerative lesions: Red, raw areas of tissue that may be painful and prone to bleeding.
- Bullous lesions: Fluid-filled blisters or vesicles that may rupture and form painful erosions.
- Diagnosis: Diagnosis of oral lichen planus is typically based on clinical examination and may involve:
- Visual inspection of the oral cavity to identify characteristic lesions.
- Biopsy of suspicious lesions for histopathological examination, which can reveal characteristic changes such as basal cell degeneration, lymphocytic infiltration, and the presence of Civatte bodies (liquefied degenerated basal cells).
- Causes: The exact cause of oral lichen planus is not fully understood, but it is believed to involve an autoimmune reaction triggered by various factors, including:
- Genetic predisposition: Certain genetic factors may increase susceptibility to developing lichen planus.
- Immune system dysfunction: Abnormal immune responses may lead to inflammation and tissue damage in the oral mucosa.
- Environmental factors: Factors such as stress, trauma, infections, medications, or allergic reactions may trigger or exacerbate lichen planus lesions.
- Treatment: Treatment of oral lichen planus aims to alleviate symptoms, reduce inflammation, and prevent complications. Management options may include:
- Topical corticosteroids: Application of corticosteroid gels, creams, or ointments directly to the affected areas to reduce inflammation and promote healing.
- Systemic corticosteroids: Oral corticosteroid medications may be prescribed for severe or widespread cases of oral lichen planus.
- Immunosuppressive agents: Medications such as cyclosporine, tacrolimus, or mycophenolate mofetil may be used to suppress immune system activity and reduce inflammation.
- Oral hygiene measures: Gentle oral hygiene practices, including regular brushing and flossing, and avoidance of irritating foods or substances.
- Symptomatic relief: Use of topical anesthetics, oral rinses, or saliva substitutes to alleviate pain, dry mouth, or discomfort associated with lichen planus lesions.
- Follow-up care: Regular monitoring by a dentist or oral medicine specialist to evaluate treatment response, monitor for disease progression, and detect any potential complications or malignant transformation.
In summary, oral lichen planus is a chronic inflammatory condition of the oral mucosa characterized by the presence of white, lacy patches, red erosions, or ulcerations. It is believed to be an autoimmune disorder with various triggers and may require a multidisciplinary approach for diagnosis and management. Treatment aims to alleviate symptoms, reduce inflammation, and improve oral health and quality of life for individuals affected by this condition.
Bridges
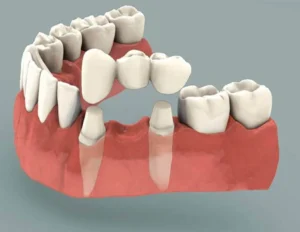
Dental bridges are fixed dental prostheses used to replace one or more missing teeth by bridging the gap between natural teeth or dental implants. They consist of one or more artificial teeth, known as pontics, which are attached to adjacent natural teeth or implants for support. Bridges are custom-made to match the color, size, and shape of the patient's natural teeth, restoring both function and aesthetics to the smile.
Here are the key aspects of dental bridges:
- Types of Bridges:
- Traditional Bridges: These are the most common type of bridges and consist of one or more pontics attached to dental crowns, which are cemented onto the natural teeth adjacent to the gap.
- Cantilever Bridges: In cases where there is only one adjacent tooth next to the gap, a cantilever bridge may be used. This type of bridge is anchored to only one natural tooth or implant.
- Maryland Bridges (Resin-Bonded Bridges): Maryland bridges use metal or porcelain wings bonded to the backs of adjacent natural teeth, eliminating the need for dental crowns. They are often used for replacing front teeth.
- Procedure:
- The process of getting a dental bridge typically involves two or more dental appointments.
- During the initial appointment, the dentist prepares the abutment teeth, which are the natural teeth adjacent to the gap, by removing a portion of their enamel to accommodate the dental crowns.
- Impressions of the prepared teeth and the surrounding dental structures are taken to fabricate the custom-made bridge in a dental laboratory.
- A temporary bridge may be placed to protect the prepared teeth while the final bridge is being fabricated.
- Once the bridge is ready, the temporary bridge is removed, and the final bridge is cemented into place, restoring function and aesthetics to the smile.
- Benefits of Dental Bridges:
- Restoration of Function: Dental bridges restore the ability to chew and speak properly, which may be compromised by missing teeth.
- Aesthetic Improvement: Bridges fill in the gaps left by missing teeth, improving the appearance of the smile and restoring facial symmetry.
- Prevention of Tooth Movement: By filling in the space left by missing teeth, bridges help prevent neighboring teeth from shifting out of position.
- Longevity: With proper care and maintenance, dental bridges can last for many years, providing a durable and cost-effective solution for tooth replacement.
- Post-Treatment Care:
- Patients with dental bridges should practice good oral hygiene habits, including brushing twice a day, flossing daily, and attending regular dental check-ups and cleanings.
- Avoiding hard or sticky foods and habits like biting on pens or fingernails can help prolong the life of the bridge and prevent damage.
- Regular monitoring by a dentist is essential to ensure the bridge remains stable and functional over time.
In summary, dental bridges offer a reliable and effective solution for replacing missing teeth, restoring both function and aesthetics to the smile. With proper care and maintenance, bridges can provide patients with a long-lasting and natural-looking tooth replacement option.