Columbia University College of Dental Medicine
Contact
Hours
- Monday: 9:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 9:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Columbia University College of Dental Medicine, located in New York, New York, is a renowned institution dedicated to excellence in dental education, research, and patient care. As one of the leading dental schools in the nation, we are committed to preparing future dental professionals through innovative educational programs, cutting-edge research initiatives, and comprehensive clinical experiences. Our faculty consists of world-class educators and researchers who are dedicated to advancing the field of dentistry and improving oral health outcomes for individuals and communities.
Educational Programs
Dental Degree Programs
- Doctor of Dental Surgery (DDS): Rigorous program designed to provide students with a comprehensive education in dental science, clinical skills, and ethical practice.
- Advanced Dental Education: Specialized postgraduate programs offering advanced training in areas such as orthodontics, periodontics, endodontics, and oral surgery.
Continuing Education
- Professional Development: Continuing education courses and seminars for practicing dentists to enhance their clinical skills, stay updated on the latest advancements in dental research, and meet licensure requirements.
- Specialized Training: Advanced training programs for dental specialists seeking to further develop their expertise in specific areas of dentistry.
Clinical Services
Patient Care
- Comprehensive Dental Care: Range of preventive, restorative, and cosmetic dental services provided by faculty-supervised students and experienced dental professionals.
- Specialty Care: Specialized treatment options for complex dental conditions, including orthodontics, periodontics, endodontics, and oral surgery.
Community Outreach
- Public Health Initiatives: Collaborative efforts with community organizations to promote oral health education, provide dental screenings, and deliver preventive services to underserved populations.
- Community Service: Participation in outreach programs and volunteer initiatives to address the oral health needs of underserved communities and improve access to dental care.
Research and Innovation
Scientific Inquiry
- Translational Research: Conducting cutting-edge research to translate scientific discoveries into clinical applications for improved patient care and outcomes.
- Interdisciplinary Collaboration: Collaborating with other academic institutions and research centers to advance knowledge in various areas of dental science and medicine.
Columbia University College of Dental Medicine is dedicated to advancing the field of dentistry through education, research, and patient care. Through our commitment to excellence and innovation, we strive to improve oral health outcomes and make a positive impact on the well-being of individuals and communities locally and globally.
Dentinogenesis Imperfecta
Dentinogenesis imperfecta (DI) is a hereditary genetic disorder that affects the development and formation of dentin, one of the primary tissues that make up teeth. It is characterized by abnormal dentin structure and composition, leading to weakened and discolored teeth that are prone to fracture, wear, and sensitivity. Dentinogenesis imperfecta is typically inherited as an autosomal dominant trait, meaning that a child has a 50% chance of inheriting the condition if one of their parents carries the mutated gene.
Here are some key points about dentinogenesis imperfecta:
- Types: Dentinogenesis imperfecta is classified into three main types based on clinical and genetic features:
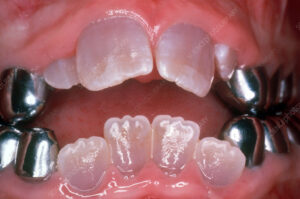
- Type I: Also known as classic or hereditary opalescent dentinogenesis imperfecta, this type is the most common and severe form of the condition. It is characterized by translucent or opalescent (bluish-gray) teeth with bulbous crowns, narrow roots, and severe attrition (wear) of the enamel. Type I DI is caused by mutations in the DSPP (dentin sialophosphoprotein) gene, which encodes a protein involved in dentin formation.
- Type II: Also known as coronal dentinogenesis imperfecta, this type is characterized by similar dental abnormalities as type I DI but with less severe enamel involvement. Teeth may appear yellow-brown or amber in color and may be more resistant to fracture compared to type I DI. Type II DI is also caused by mutations in the DSPP gene.
- Type III: Also known as Brandywine type dentinogenesis imperfecta, this type is characterized by similar dental abnormalities as type II DI but with additional skeletal abnormalities such as short stature and joint laxity. Type III DI is caused by mutations in the DSPP gene as well.
- Clinical Presentation: Dentinogenesis imperfecta typically presents with a distinctive appearance of the teeth, including opalescent or discolored enamel, bulbous crowns, and attrition of the enamel exposing the underlying dentin. The teeth may appear translucent or amber in color, and the enamel may chip or fracture easily due to its weakened structure. Individuals with dentinogenesis imperfecta may also experience dental sensitivity, pulp exposure, and increased risk of dental caries and infections.
- Diagnosis: Diagnosis of dentinogenesis imperfecta is based on clinical and radiographic findings, including characteristic dental abnormalities such as opalescent or discolored enamel, bulbous crowns, and narrowed pulp chambers. Dental X-rays may reveal thin and bulbous roots, obliteration of the pulp chambers, and dentin defects such as taurodontism (enlarged pulp chambers) or pulpal calcifications. Genetic testing may be performed to confirm the diagnosis and identify the underlying genetic mutation responsible for the condition.
- Treatment: Treatment of dentinogenesis imperfecta focuses on preserving tooth structure, preventing complications, and improving oral function and aesthetics. Management options may include dental restorations such as crowns, veneers, or composite fillings to protect and reinforce weakened teeth, extraction of severely affected teeth followed by prosthetic replacement, endodontic therapy (root canal treatment) for teeth with pulp exposure or infection, and preventive measures such as fluoride therapy and meticulous oral hygiene to reduce the risk of dental caries and infections.
In summary, dentinogenesis imperfecta is a hereditary genetic disorder characterized by abnormal development and structure of dentin, resulting in weakened and discolored teeth that are prone to fracture, wear, and sensitivity. Early diagnosis and appropriate dental management are essential for preserving tooth structure, preventing complications, and improving oral function and aesthetics in individuals with dentinogenesis imperfecta.
Oral Submucous Fibrosis
Oral submucous fibrosis (OSMF) is a chronic, progressive, potentially malignant disorder that affects the oral mucosa, particularly the buccal mucosa (inner lining of the cheeks) and other soft tissues of the mouth. It is characterized by fibrosis (formation of scar tissue) and progressive stiffness of the oral mucosa, resulting in restricted mouth opening (trismus) and difficulty in eating, speaking, and maintaining oral hygiene. OSMF is most commonly associated with the habit of betel nut (areca nut) chewing, particularly in regions where betel quid chewing is prevalent, such as South Asia and Southeast Asia.
Here are some key points about oral submucous fibrosis:
- Etiology: The exact cause of oral submucous fibrosis is not fully understood, but it is believed to result from chronic irritation and inflammation of the oral mucosa, particularly due to the habit of betel nut chewing. Betel nut contains arecoline, a potent vasoconstrictor and fibrogenic agent that can induce fibrosis and collagen deposition in the oral tissues. Other factors implicated in the pathogenesis of OSMF include the use of tobacco, spicy foods, nutritional deficiencies, genetic predisposition, and immunological factors.
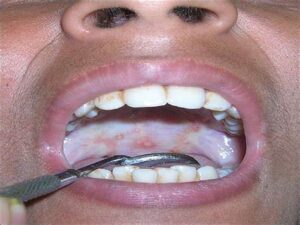
- Clinical Presentation: Oral submucous fibrosis typically presents as a progressive, insidious fibrosis of the oral mucosa, initially manifesting as blanching or whitening of the buccal mucosa and soft palate. As the condition progresses, the fibrosis extends to involve other oral tissues, leading to loss of elasticity, reduced mouth opening (trismus), and palpable fibrous bands or ridges along the buccal mucosa and posterior pharyngeal wall. Patients may experience difficulty in mouth opening, altered sensation or numbness in the oral mucosa, burning or tingling sensation, and impaired taste sensation.
- Diagnosis: Diagnosis of oral submucous fibrosis is based on clinical examination, history of betel nut or tobacco use, and characteristic features such as blanching of the oral mucosa, palpable fibrous bands, and reduced mouth opening. In advanced cases, imaging studies such as panoramic radiography or computed tomography (CT) may be performed to assess the extent of fibrosis and rule out complications such as oral cancer. Biopsy may be indicated to confirm the diagnosis and rule out malignancy in suspicious lesions.
- Treatment: Treatment of oral submucous fibrosis aims to alleviate symptoms, prevent disease progression, and improve oral function and quality of life. Management options may include cessation of betel nut and tobacco use, dietary modification (avoidance of spicy or irritant foods), oral hygiene measures, and symptomatic treatment of pain or discomfort. In cases of moderate to severe fibrosis or trismus, interventions such as intralesional corticosteroid injections, physiotherapy, oral splints, or surgical release of fibrous bands may be considered to improve mouth opening and relieve symptoms.
- Complications: Complications of oral submucous fibrosis include increased risk of oral cancer, particularly squamous cell carcinoma, due to the malignant transformation of fibrotic oral mucosa. Patients with OSMF should be closely monitored for signs of malignant transformation, such as ulceration, induration, or non-healing lesions, and referred for further evaluation and management if necessary.
In summary, oral submucous fibrosis is a chronic, potentially malignant disorder characterized by fibrosis and stiffness of the oral mucosa, resulting in restricted mouth opening and difficulty in eating, speaking, and maintaining oral hygiene. The condition is most commonly associated with betel nut chewing and requires early diagnosis and appropriate management to prevent disease progression and complications such as oral cancer. Interventional measures aimed at reducing or eliminating the causative factors and improving oral function are essential for the long-term management of oral submucous fibrosis.