Kids Only Dental
Contact
Hours
- Monday: 1:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 1:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Kids Only Dental, located in New York, NY, is a premier pediatric dental practice dedicated exclusively to the dental needs of children. The clinic is known for its child-friendly environment, state-of-the-art facilities, and a team of highly trained animal dental professionals who provide compassionate and specialized care to ensure a positive dental experience for every child.
Dental Services
Preventive Dentistry
- Comprehensive Oral Exams: Thorough examinations to monitor and maintain oral health, with a focus on early detection of dental issues.
- Routine Cleanings: Regular cleanings to prevent cavities and promote healthy teeth and gums.
- Fluoride Treatments: Strengthening treatments to protect children’s teeth from decay.
- Dental Sealants: Protective coatings applied to the chewing surfaces of molars to prevent cavities.
Specialized Pediatric Dental Care
- Restorative Dentistry: Fillings and crowns to repair cavities and restore damaged teeth in children.
- Orthodontic Assessments: Early evaluations and referrals for orthodontic treatment to correct dental alignment and bite issues.
- Emergency Dental Care: Prompt and effective treatment for dental emergencies, such as toothaches, broken teeth, or dental trauma.
- Behavior Management: Techniques to help children feel comfortable and at ease during dental visits, including sedation dentistry options for anxious patients.
Educational Programs
- Oral Hygiene Education: Teaching children proper brushing and flossing techniques to encourage good oral hygiene habits.
- Nutrition Counseling: Guidance on healthy eating habits that support dental health.
- Parental Support: Resources and advice for parents to help them care for their children’s dental needs at home.
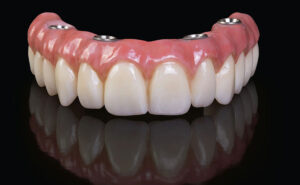
All-on-4 Dental Implants
"All-on-4" dental implants refer to a specific dental implant treatment concept designed to provide edentulous (toothless) patients with a fixed full-arch dental restoration supported by only four dental implants. This innovative treatment approach allows for the rehabilitation of an entire dental arch (either upper or lower) using fewer implants compared to traditional implant-supported prostheses. Here's an overview of the All-on-4 dental implant procedure:
- Evaluation and Treatment Planning:
- Before undergoing All-on-4 dental implant treatment, the patient will undergo a comprehensive dental examination, including clinical assessment and radiographic evaluation (such as dental X-rays or CBCT scans).
- The dentist or oral surgeon will assess the patient's oral health, bone density, and suitability for implant placement.
- A detailed treatment plan will be developed based on the patient's individual needs and goals.
- Implant Placement:
- The first step in the All-on-4 dental implant procedure involves surgically placing four dental implants into the jawbone at strategic locations to support the full-arch restoration.
- The implants are strategically angled and positioned to maximize bone anchorage and avoid anatomical structures, such as nerves or sinuses.
- Implant placement is typically performed under local anesthesia or sedation to ensure the patient's comfort during the procedure.
- Immediate Loading:
- In many cases, All-on-4 dental implants allow for immediate loading, meaning that a temporary fixed prosthesis can be attached to the implants on the same day as surgery.
- Immediate loading provides patients with immediate function and aesthetics while the implants undergo osseointegration.
- Healing and Osseointegration:
- After implant placement, a healing period of several months is usually required to allow for osseointegration to occur.
- During this time, the implants fuse with the surrounding bone tissue, becoming firmly anchored in the jawbone.
- Temporary restorations may be placed during the healing period to maintain aesthetics and function.
- Final Restoration:
- Once osseointegration is complete, the dental implants are ready to support the final full-arch restoration.
- A custom-made fixed prosthesis, typically made of high-quality dental materials such as porcelain or acrylic, is fabricated to fit securely over the implants and restore function and aesthetics.
- The final prosthesis is attached to the implants using special abutments or connectors, providing stability and support for chewing and speaking.
- Postoperative Care and Maintenance:
- After the All-on-4 dental implant restoration is placed, the patient will receive instructions on postoperative care and maintenance.
- Regular dental check-ups and professional cleanings are essential to monitor the health of the implants and surrounding tissues.
- Good oral hygiene practices, including brushing, flossing, and using antimicrobial mouthwash, are important for long-term success.
All-on-4 dental implants offer several advantages over traditional removable dentures, including improved stability, function, and aesthetics. With proper care and maintenance, an All-on-4 dental implant restoration can provide long-lasting and natural-looking results, enhancing both oral health and quality of life. If you are considering All-on-4 dental implant treatment, it's important to consult with a qualified dental professional to determine the best treatment plan for your individual needs.
Tooth Impaction
Tooth impaction occurs when a tooth fails to erupt properly through the gum tissue into its normal functional position within the dental arch. This condition is common for third molars (wisdom teeth) but can also affect other teeth, including canines and premolars. Tooth impaction can lead to various dental problems and may require intervention to prevent complications.
Here are some key points about tooth impaction:
- Causes: Tooth impaction can occur due to various factors, including:
- Insufficient space: Lack of adequate space within the dental arch can prevent a tooth from erupting properly.
- Malposition: Abnormal tooth positioning or angulation may hinder the tooth's ability to erupt into its proper alignment.
- Overcrowding: Crowding of teeth within the dental arch can impede the eruption of one or more teeth.
- Delayed eruption: Developmental abnormalities or genetic factors may delay the eruption of teeth, leading to impaction.
- Obstruction: Physical barriers such as cysts, tumors, or adjacent teeth may obstruct the path of eruption and result in impaction.
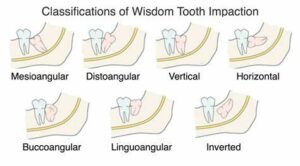
- Types of Tooth Impaction:
- Soft tissue impaction: The tooth is partially covered by the gum tissue and cannot fully erupt into the oral cavity.
- Partial bony impaction: The tooth is partially covered by bone tissue, limiting its eruption into the oral cavity.
- Complete bony impaction: The tooth is fully encased within the jawbone and cannot erupt into the oral cavity.
- Commonly Impacted Teeth:
- Wisdom teeth (third molars): Wisdom teeth are frequently impacted due to their late eruption and limited space within the dental arch.
- Canine teeth (maxillary and mandibular): Canine teeth, also known as cuspids, may become impacted due to their important role in occlusion and alignment.
- Premolars: Premolar teeth may become impacted, particularly in cases of overcrowding or abnormal tooth development.
- Symptoms:
- Symptoms of tooth impaction may vary depending on the severity and location of the impacted tooth.
- Common symptoms may include pain, swelling, and tenderness in the affected area.
- Difficulty chewing or biting, particularly if the impacted tooth interferes with occlusion.
- Sensitivity or discomfort when brushing or flossing around the impacted tooth.
- Complications:
- Tooth decay (caries): Impacted teeth may be more difficult to clean effectively, increasing the risk of tooth decay and cavities.
- Gum disease (periodontal disease): Difficulty maintaining proper oral hygiene around impacted teeth may lead to gum inflammation and periodontal problems.
- Cyst or tumor formation: Impacted teeth can sometimes develop cysts or tumors within the jawbone, which may require surgical intervention.
- Tooth crowding or misalignment: Impacted teeth may exert pressure on adjacent teeth, causing crowding or shifting of teeth within the dental arch.
- Treatment:
- Treatment of tooth impaction depends on various factors, including the type and severity of impaction, the position of the impacted tooth, and the presence of symptoms or complications.
- Treatment options may include:
- Observation and monitoring: In some cases, asymptomatic impacted teeth may be monitored closely without immediate intervention.
- Extraction: Surgical removal of the impacted tooth may be recommended to alleviate symptoms, prevent complications, and preserve oral health.
- Orthodontic treatment: Orthodontic techniques such as braces or clear aligners may be used to create space within the dental arch and facilitate the eruption of impacted teeth into their proper alignment.
- Surgical exposure and orthodontic traction: In cases of impacted canines or premolars, surgical exposure of the impacted tooth followed by orthodontic traction may be performed to guide the tooth into its correct position within the dental arch.
In summary, tooth impaction occurs when a tooth fails to erupt properly into its normal functional position within the dental arch. This condition can lead to various dental problems and may require intervention to prevent complications. Treatment options for tooth impaction depend on factors such as the type and severity of impaction, presence of symptoms or complications, and individual patient considerations. Early diagnosis and appropriate management are essential for preserving oral health and preventing long-term complications associated with tooth impaction.