New York Endodontic Associates
Contact
Hours
<ul id=”hours” style=”transition: height .3s ease;”>
<li>Monday: 9:00am – 9:00pm</li>
<li>Tuesday: 9:00am – 6:00pm</li>
<li>Wednesday: 9:00am – 9:00pm</li>
<li>Thursday: 9:00am – 9:00pm</li>
<li>Friday: 9:00am – 5:00pm</li>
</ul>
New York Endodontic Associates, located in the bustling city of New York, NY, is a leading practice specializing in endodontic care. The practice is dedicated to providing exceptional root canal therapy and other endodontic treatments in a comfortable and compassionate environment. Led by a team of experienced endodontists, New York Endodontic Associates offers state-of-the-art procedures to save natural teeth and relieve dental pain.
Endodontic Services
Root Canal Therapy
- Expert Diagnosis: Accurate diagnosis of dental pain and identification of the cause to determine the need for root canal treatment.
- Precision Treatment: State-of-the-art techniques and equipment to perform root canal therapy with precision and efficiency.
- Gentle Care: Compassionate approach to alleviate dental anxiety and ensure a comfortable experience for every patient.
Endodontic Surgery
- Apicoectomy: Surgical procedure to remove infected tissue and seal the root tip, often performed when conventional root canal therapy is not sufficient.
- Root Canal Retreatment: Revision of a previous root canal treatment to address persistent infection or other complications.
Advanced Procedures
Microscopic Endodontics
- High-Powered Microscopes: Utilization of advanced microscopes for enhanced visualization and precision during root canal procedures.
- Ultrasonic Instrumentation: Gentle and efficient removal of infected tissue using ultrasonic technology, minimizing trauma to surrounding tissues.
Regenerative Endodontics
- Pulpotomy: Partial removal of damaged pulp tissue followed by application of regenerative materials to promote healing and preserve tooth vitality.
- Revascularization: Stimulating the growth of new blood vessels and tissues inside the tooth to revitalize damaged or infected pulp.
Patient Care
Comprehensive Consultations
- Thorough Examinations: Detailed evaluations and discussions to educate patients about their treatment options and address any concerns.
- Personalized Treatment Plans: Customized treatment plans tailored to each patient’s unique oral health needs and goals.
Comfort and Support
- Relaxing Environment: A calming atmosphere designed to help patients feel at ease during their visits.
- Pain Management: Utilization of advanced anesthesia techniques to minimize discomfort during procedures.
Oral Thrush
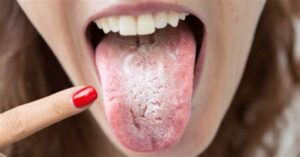
Oral thrush, also known as oral candidiasis, is a fungal infection caused by Candida yeast species, typically Candida albicans. It commonly affects the mouth and throat, particularly the mucous membranes and moist areas such as the tongue, inner cheeks, gums, and throat. Oral thrush can cause discomfort, pain, and difficulty swallowing, and it is more prevalent in individuals with weakened immune systems, certain medical conditions, or those taking medications that disrupt the balance of microorganisms in the mouth.
Here are some key points about oral thrush:
- Causes:
- Candida overgrowth: Oral thrush occurs when there is an overgrowth of Candida yeast in the mouth, often due to factors that disrupt the natural balance of microorganisms in the oral cavity.
- Weakened immune system: Conditions that weaken the immune system, such as HIV/AIDS, diabetes, cancer, or autoimmune disorders, increase the risk of oral thrush.
- Medications: Certain medications, such as antibiotics, corticosteroids, immunosuppressants, or chemotherapy drugs, can alter the oral microbiota and predispose individuals to oral thrush.
- Hormonal changes: Hormonal fluctuations, such as those occurring during pregnancy, menopause, or hormonal therapy, can increase susceptibility to oral thrush.
- Poor oral hygiene: Inadequate oral hygiene practices, such as infrequent brushing, flossing, or denture cleaning, can contribute to the development of oral thrush.
- Smoking: Tobacco use, particularly smoking, can weaken the immune system and promote Candida overgrowth in the mouth.
- Symptoms:
- White, creamy, or yellowish patches on the tongue, inner cheeks, gums, or throat.
- Soreness, burning, or discomfort in the mouth, especially when eating or drinking.
- Difficulty swallowing or persistent throat pain.
- Loss of taste or altered taste sensation (dysgeusia).
- Cracking or redness at the corners of the mouth (angular cheilitis) in severe cases.
- Bleeding or mucosal irritation when the patches are scraped or rubbed.
- Diagnosis:
- Diagnosis of oral thrush is typically based on clinical examination and evaluation of symptoms by a healthcare professional.
- Your healthcare provider may perform a physical examination of the mouth and throat and may collect samples (swabs) from the affected areas for microscopic examination or culture to confirm the presence of Candida yeast.
- Treatment:
- Treatment of oral thrush aims to eliminate the fungal infection, alleviate symptoms, and prevent recurrence. Treatment options may include:
- Antifungal medications: Topical antifungal agents such as nystatin oral suspension or clotrimazole lozenges are commonly used to treat mild to moderate cases of oral thrush. Severe or persistent infections may require systemic antifungal medications such as fluconazole.
- Oral hygiene measures: Practicing good oral hygiene, including regular brushing, flossing, and tongue cleaning, can help reduce oral thrush symptoms and prevent recurrence.
- Denture care: Proper cleaning and maintenance of dentures or oral appliances are essential to prevent Candida overgrowth and denture-related oral thrush.
- Treatment of underlying conditions: Managing underlying medical conditions or risk factors such as diabetes, immunosuppression, or hormonal imbalances is important to prevent recurrent episodes of oral thrush.
- Prevention:
- To prevent oral thrush, it's important to:
- Maintain good oral hygiene practices, including regular brushing, flossing, and tongue cleaning.
- Limit sugar and yeast-containing foods in the diet, as these can promote Candida overgrowth.
- Use antibiotics judiciously and only as prescribed by a healthcare professional to minimize disruption of the oral microbiota.
- Avoid smoking or tobacco use, as these can weaken the immune system and increase susceptibility to oral thrush.
- Practice proper denture care, including regular cleaning, soaking, and removal at night to allow the oral tissues to breathe.
In summary, oral thrush is a fungal infection caused by Candida yeast species that commonly affects the mouth and throat. It can cause discomfort, pain, and difficulty swallowing, particularly in individuals with weakened immune systems or certain medical conditions. Treatment of oral thrush typically involves antifungal medications, oral hygiene measures, and management of underlying conditions to alleviate symptoms and prevent recurrence. If you suspect you have oral thrush or experience persistent symptoms such as white patches in the mouth or throat, it's important to consult a healthcare professional for evaluation and appropriate treatment.
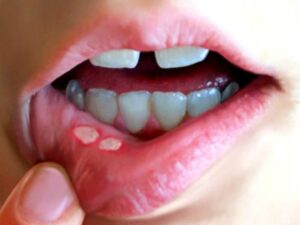
Stomatitis
Stomatitis refers to the inflammation of the mucous lining inside the mouth. This condition can occur due to various factors, including infections (viral, bacterial, or fungal), irritants (such as tobacco or alcohol), autoimmune disorders, or certain medications. Symptoms of stomatitis may include pain, redness, swelling, ulcers, and difficulty eating or swallowing. Treatment typically involves addressing the underlying cause and managing symptoms with pain relief medications, topical ointments, or antimicrobial agents. Maintaining good oral hygiene and avoiding known irritants can help prevent stomatitis from recurring. If you're experiencing persistent mouth discomfort or suspect you have stomatitis, it's important to seek medical advice for proper diagnosis and treatment.