Stony Brook School of Dental Medicine
Contact
Hours
- Monday: 9:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 9:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Stony Brook School of Dental Medicine, located in Stony Brook, New York, is a prestigious institution committed to excellence in dental education, research, and patient care. As a leading dental school, we are dedicated to preparing the next generation of dental professionals through innovative educational programs, cutting-edge research initiatives, and comprehensive clinical experiences. Our faculty consists of renowned experts in the field of dentistry who are committed to advancing oral health and providing exceptional care to patients.
Educational Programs
Dental Degree Programs
- Doctor of Dental Surgery (DDS): Rigorous program designed to provide students with a solid foundation in dental science, clinical skills, and professional ethics.
- Advanced Dental Education: Specialized postgraduate programs offering advanced training in areas such as orthodontics, periodontics, endodontics, and oral surgery.
Continuing Education
- Professional Development: Continuing education courses and seminars for practicing dentists to stay abreast of the latest advancements in dental research, technology, and clinical practice.
- Specialized Training: Advanced training programs for dental specialists seeking to enhance their skills and expertise in specific areas of dentistry.
Clinical Services
Patient Care
- Comprehensive Dental Care: Range of preventive, restorative, and cosmetic dental services provided by faculty-supervised students and experienced dental professionals.
- Specialty Care: Specialized treatment options for complex dental issues, including orthodontics, periodontics, endodontics, and oral surgery.
Community Outreach
- Public Health Initiatives: Collaborative efforts with community organizations to promote oral health education, provide dental screenings, and deliver preventive services to underserved populations.
- Community Service: Participation in outreach programs and volunteer initiatives to address the oral health needs of local communities and improve access to dental care.
Research and Innovation
Scientific Inquiry
- Translational Research: Conducting innovative research to translate scientific discoveries into clinical applications for improved patient care and outcomes.
- Interdisciplinary Collaboration: Collaborating with other academic institutions and research centers to advance knowledge in various areas of dental science and medicine.
Stony Brook School of Dental Medicine is dedicated to excellence in dental education, patient care, and research, serving the needs of individuals and communities in Stony Brook and beyond. Through our commitment to academic excellence, clinical innovation, and community engagement, we strive to make a positive impact on the oral health and well-being of society.
Apicoectomy
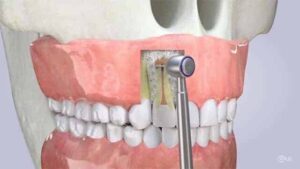
Apicoectomy, also known as root-end resection or root-end surgery, is a dental surgical procedure performed to remove the tip of the tooth's root (apex) and any infected tissue surrounding it. This procedure is typically indicated when a conventional root canal treatment has failed to resolve persistent infection or inflammation in the root canal system of a tooth.
Here's an overview of the apicoectomy procedure:
- Indications:
- Apicoectomy is indicated when a tooth that has undergone root canal treatment continues to exhibit signs of infection, inflammation, or persistent symptoms such as pain, swelling, or drainage.
- Common reasons for apicoectomy include the presence of infection or inflammation in the root canal system that cannot be resolved with conventional root canal therapy, persistent periapical lesions (abscesses), or the presence of accessory canals or anatomical complexities that cannot be adequately treated with nonsurgical means.
- Preoperative Assessment:
- Before performing an apicoectomy, the dentist or endodontist will conduct a comprehensive evaluation of the affected tooth, including clinical examination, radiographic assessment (X-rays), and possibly additional diagnostic tests such as pulp vitality testing or cone-beam computed tomography (CBCT).
- The goal of the preoperative assessment is to identify the cause of the persistent infection or inflammation and determine the suitability of apicoectomy as a treatment option.
- Procedure:
- Anesthesia: Local anesthesia is administered to numb the area surrounding the affected tooth and ensure the patient's comfort during the procedure.
- Tooth isolation: The tooth and surrounding area are isolated using a dental dam or other protective barrier to maintain a clean and sterile field.
- Access: The dentist or endodontist makes a small incision in the gum tissue near the apex of the tooth to access the underlying bone and root tip.
- Root-end resection: Using specialized dental instruments, the dentist or endodontist removes the tip of the tooth's root (apex) along with any infected or inflamed tissue.
- Root-end preparation: The root canal(s) of the tooth may be cleaned, shaped, and filled with a biocompatible material to seal the root canal space and prevent recontamination or reinfection.
- Root-end sealing: A small filling material (such as gutta-percha) is placed in the prepared root canal space, and a root-end filling material (such as mineral trioxide aggregate or dental cement) is used to seal the root-end cavity.
- Suture placement: The gum tissue is repositioned and sutured back into place to facilitate healing.
- Postoperative Care:
- Following the procedure, the patient may experience some discomfort, swelling, or bruising, which can be managed with pain medication and cold compresses applied to the outside of the cheek.
- Patients are advised to follow postoperative instructions provided by the dentist or endodontist, including dietary restrictions, oral hygiene practices, and any prescribed medications.
- Regular follow-up appointments are scheduled to monitor healing, assess the success of the procedure, and address any concerns or complications.
- Prognosis:
- The success of apicoectomy depends on various factors, including the extent of infection or inflammation, the quality of the root-end preparation and sealing, and the patient's oral hygiene and compliance with postoperative care instructions.
- With proper care and maintenance, apicoectomy can provide a favorable outcome, relieving symptoms and preserving the affected tooth for long-term function and aesthetics.
In summary, apicoectomy is a dental surgical procedure performed to remove the tip of a tooth's root (apex) and any infected tissue surrounding it, typically indicated when conventional root canal treatment has failed to resolve persistent infection or inflammation. If you have a tooth that may require apicoectomy or if you have any questions about the procedure, it's important to consult with your dentist or endodontist for a thorough evaluation and personalized treatment plan.
Burning Mouth Syndrome
Burning mouth syndrome (BMS) is a complex and often frustrating condition characterized by a burning sensation or discomfort in the mouth, typically involving the tongue, lips, palate, gums, or throat. The discomfort may range from mild to severe and may persist for months or even years. BMS can significantly impact quality of life and may lead to difficulty eating, speaking, and performing daily activities.
Here are some key points about burning mouth syndrome:
- Symptoms:
- Burning or scalding sensation in the mouth, often described as a feeling of heat, tingling, or numbness.
- Dry mouth (xerostomia) or excessive saliva production (sialorrhea).
- Altered taste sensation, such as a metallic or bitter taste.
- Soreness or irritation of the mouth tissues, including the tongue, lips, gums, palate, or throat.
- Symptoms may worsen throughout the day, peaking in the late afternoon or evening.
- Causes:
- The exact cause of burning mouth syndrome is often difficult to determine and may involve multiple factors.
- Potential causes or contributing factors may include:
- Oral candidiasis (yeast infection), oral thrush, or other oral infections.
- Dry mouth (xerostomia) due to reduced saliva production, which can be caused by medications, systemic conditions, or salivary gland dysfunction.
- Nutritional deficiencies, such as vitamin B12 deficiency, iron deficiency, or folate deficiency.
- Hormonal changes, particularly in women during menopause or hormonal fluctuations.
- Psychological factors, such as stress, anxiety, depression, or psychological disorders.
- Neurological disorders or nerve damage, such as trigeminal neuralgia or neuropathic pain syndromes.
- Allergic reactions or sensitivity to certain foods, food additives, dental materials, or oral hygiene products.
- Diagnosis:
- Diagnosis of burning mouth syndrome involves a comprehensive evaluation by a healthcare provider, typically a dentist, oral medicine specialist, or otolaryngologist.
- Medical and dental history, including medication use, dietary habits, oral hygiene practices, and presence of underlying medical conditions or psychological factors.
- Clinical examination of the oral cavity, including assessment of oral mucosa, salivary gland function, and presence of oral infections or lesions.
- Laboratory tests, such as blood tests to assess for nutritional deficiencies or systemic conditions, and oral swabs or cultures to evaluate for oral infections.
- Treatment:
- Treatment of burning mouth syndrome aims to alleviate symptoms, address underlying causes or contributing factors, and improve quality of life.
- Management options may include:
- Symptomatic relief measures, such as topical oral analgesics, mouth rinses, or oral moisturizers to soothe and hydrate the oral tissues.
- Medications, such as tricyclic antidepressants, anticonvulsants, benzodiazepines, or topical capsaicin, to manage neuropathic pain or underlying psychological factors.
- Correction of nutritional deficiencies through dietary modifications or supplementation with vitamins or minerals.
- Stress management techniques, relaxation therapies, or counseling to address psychological factors contributing to symptoms.
- Avoidance of potential triggers or irritants, such as spicy foods, acidic beverages, tobacco, alcohol, or irritating oral hygiene products.
- Referral to specialists, such as oral medicine specialists, neurologists, or psychologists, for further evaluation and management of underlying conditions.
- Prognosis:
- The prognosis for burning mouth syndrome varies depending on the underlying cause, severity of symptoms, and response to treatment.
- Some individuals may experience spontaneous resolution or improvement of symptoms over time, while others may require ongoing management and support.
- Multidisciplinary approach involving dental, medical, and psychological interventions may be necessary for comprehensive management of burning mouth syndrome.
In summary, burning mouth syndrome is a complex and often challenging condition characterized by a burning sensation or discomfort in the mouth. It can have multiple potential causes or contributing factors and may require a comprehensive evaluation and management approach involving dental, medical, and psychological interventions. Treatment aims to alleviate symptoms, address underlying causes, and improve quality of life for individuals affected by this condition.