Touro College of Dental Medicine
Contact
Hours
- Monday: 9:00am – 9:00pm
- Tuesday: 9:00am – 6:00pm
- Wednesday: 9:00am – 9:00pm
- Thursday: 9:00am – 9:00pm
- Friday: 9:00am – 5:00pm
Touro College of Dental Medicine, located in New York, New York, is a distinguished institution dedicated to providing exceptional dental education, advancing research in the field of dentistry, and delivering compassionate patient care. As a leading dental school, we are committed to preparing competent and compassionate dental professionals who will serve their communities with integrity and excellence. Our faculty comprises esteemed educators and researchers who are passionate about fostering the next generation of dental leaders and advancing oral health for all.
Educational Programs
Dental Degree Programs
- Doctor of Dental Surgery (DDS): Comprehensive program designed to provide students with a solid foundation in dental science, clinical skills, and professional ethics.
- Advanced Dental Education: Postgraduate programs offering specialized training in areas such as orthodontics, periodontics, endodontics, and oral surgery.
Continuing Education
- Professional Development: Continuing education courses and seminars for practicing dentists to enhance their clinical skills, stay updated on the latest advancements in dental research, and meet licensure requirements.
- Specialized Training: Advanced training programs for dental specialists seeking to further develop their expertise in specific areas of dentistry.
Clinical Services
Patient Care
- Comprehensive Dental Care: Range of preventive, restorative, and cosmetic dental services provided by faculty-supervised students and experienced dental professionals.
- Specialty Care: Specialized treatment options for complex dental conditions, including orthodontics, periodontics, endodontics, and oral surgery.
Community Outreach
- Public Health Initiatives: Collaborative efforts with community organizations to promote oral health education, provide dental screenings, and deliver preventive services to underserved populations.
- Community Service: Participation in outreach programs and volunteer initiatives to address the oral health needs of underserved communities and improve access to dental care.
Research and Innovation
Scientific Inquiry
- Translational Research: Conducting cutting-edge research to translate scientific discoveries into clinical applications for improved patient care and outcomes.
- Interdisciplinary Collaboration: Collaborating with other academic institutions and research centers to advance knowledge in various areas of dental science and medicine.
Touro College of Dental Medicine is dedicated to excellence in dental education, research, and patient care, serving the needs of individuals and communities in New York and beyond. Through our commitment to academic excellence, clinical innovation, and community engagement, we strive to make a positive impact on oral health and well-being for generations to come.
Anesthesia
Dental anesthesia, also known as dental anesthetic or local anesthesia, is a medication used by dentists to numb specific areas of the mouth and surrounding tissues during dental procedures. It helps to alleviate pain and discomfort, allowing the dentist to perform treatments effectively and comfortably for the patient.
Here's how dental anesthesia typically works:
- Application: Dental anesthesia is usually administered via injection directly into the gums or tissues near the area being treated. Before administering the injection, the dentist may apply a topical anesthetic gel or spray to numb the surface of the skin and minimize the discomfort of the injection.
- Numbing Effect: Once injected, the anesthesia begins to take effect within a few minutes, temporarily blocking nerve signals in the affected area and preventing the sensation of pain. The patient may feel a tingling or numbing sensation as the anesthesia takes effect, but they should not experience any pain during the procedure.
- Duration: The duration of dental anesthesia varies depending on the type and concentration of the anesthetic used, as well as individual factors such as metabolism and sensitivity to the medication. In general, the effects of local anesthesia typically last for several hours, providing adequate pain relief during and after the dental procedure.
- Types of Anesthesia: There are different types of dental anesthesia available, including lidocaine, articaine, mepivacaine, and prilocaine, among others. The dentist will select the most appropriate type of anesthesia based on the specific needs of the patient and the nature of the dental treatment.
- Safety: Dental anesthesia is considered safe when administered by trained dental professionals in appropriate doses and concentrations. However, like any medication, it carries some risks and potential side effects, such as numbness, swelling, bruising, or allergic reactions. Patients should inform their dentist about any allergies, medical conditions, or medications they are taking before receiving anesthesia.
Dental anesthesia plays a crucial role in ensuring patient comfort and safety during dental procedures, allowing dentists to perform treatments efficiently and effectively. By numbing the affected area and minimizing pain, anesthesia helps to reduce anxiety and fear associated with dental visits, making the experience more pleasant for the patient. Patients should feel free to discuss any concerns or questions they have about dental anesthesia with their dentist before undergoing treatment.
Frenectomy
A frenectomy is a surgical procedure performed to remove or release a frenulum, a small fold of tissue that connects two structures in the body. In dentistry, frenectomy most commonly refers to the removal or modification of the lingual frenulum (the band of tissue connecting the underside of the tongue to the floor of the mouth) or the labial frenulum (the band of tissue connecting the lips to the gums).
Here's an overview of the frenectomy procedure:
- Indications:
- Lingual frenectomy may be indicated when the lingual frenulum is too short, tight, or thick, resulting in restricted movement of the tongue (a condition known as ankyloglossia or tongue-tie). This restriction can interfere with speech, eating, and oral hygiene.
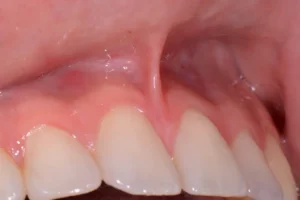
- Labial frenectomy may be indicated when the labial frenulum is attached too close to the gumline, causing tension or pulling on the gums. This can contribute to gum recession, difficulty in maintaining oral hygiene, and aesthetic concerns.
- Preparation:
- Before performing a frenectomy, the dentist or oral surgeon will conduct a clinical examination to assess the extent of the frenulum attachment and evaluate the patient's oral health.
- Local anesthesia may be administered to numb the area and ensure the patient's comfort during the procedure.
- Procedure:
- Lingual frenectomy: The dentist or oral surgeon uses a scalpel, laser, or other surgical instrument to make an incision in the lingual frenulum, effectively releasing the attachment. The tissue is then carefully dissected and removed.
- Labial frenectomy: A similar technique is used to release the attachment of the labial frenulum from the gumline. The tissue is excised to allow for proper movement and positioning of the lips.
- Postoperative Care:
- After the frenectomy procedure, the patient may experience some discomfort, swelling, or mild bleeding in the surgical area. Pain medication and cold compresses may be recommended to alleviate discomfort and reduce swelling.
- The patient should follow postoperative instructions provided by the dentist or oral surgeon, including dietary restrictions, oral hygiene practices, and any prescribed medications.
- Healing typically occurs within a few days to a week, depending on the extent of the procedure and the individual's healing response.
- Follow-up:
- Follow-up appointments may be scheduled to monitor healing and ensure proper function and mobility of the affected area.
- Speech therapy or exercises may be recommended to optimize tongue movement and function, especially in cases of lingual frenectomy for tongue-tie.
Frenectomy is a relatively simple and straightforward procedure with low risk and high success rates. It can significantly improve oral function, speech, and oral hygiene in patients with restricted frenula. If you or your child are experiencing symptoms related to a tight or restrictive frenulum, it's important to consult with a qualified dental professional for an evaluation and personalized treatment plan.